What is Diverticulosis?
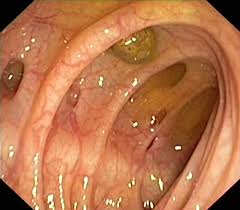
A diverticulum is defined as a pouch in the intestinal wall. All areas of the intestine can have diverticulae except the rectum. The area that is most commonly discussed in the clinical context however is diverticular disease of the colon; specifically the sigmoid colon.
The presence of diverticulae in the colon is known as diverticulosis or diverticular disease. Diverticulitis is a syndrome associated with an inflammatory reaction of the bowel wall secondary to a microscopic perforation in a diverticulum.
The incidence of diverticular disease increases significantly with age and symptomatic diverticular disease is rare before age 40. By age 80, up to two thirds of the population will have diverticular disease. Men and women are both affected equally, but it is much more common in areas where dietary fibre intake is low (like North America).
The vast majority of people with diverticular disease will never have symptoms attributable to the diverticular area. Of those that have symptoms, the two most common symptoms are diverticulitis (inflammation of the diverticular area) and bleeding. People with Irritable Bowel Syndrome have an equal incidence of diverticulosis as they age and it is important to try to separate symptoms in these patients before deciding on a treatment plan.
For more discussion of diverticular disease click here .
The presence of diverticulae in the colon is known as diverticulosis or diverticular disease. Diverticulitis is a syndrome associated with an inflammatory reaction of the bowel wall secondary to a microscopic perforation in a diverticulum.
The incidence of diverticular disease increases significantly with age and symptomatic diverticular disease is rare before age 40. By age 80, up to two thirds of the population will have diverticular disease. Men and women are both affected equally, but it is much more common in areas where dietary fibre intake is low (like North America).
The vast majority of people with diverticular disease will never have symptoms attributable to the diverticular area. Of those that have symptoms, the two most common symptoms are diverticulitis (inflammation of the diverticular area) and bleeding. People with Irritable Bowel Syndrome have an equal incidence of diverticulosis as they age and it is important to try to separate symptoms in these patients before deciding on a treatment plan.
For more discussion of diverticular disease click here .
Diverticulitis
The most common symptom of diverticulitis is pain in the left lower portion of the abdomen. There may be associated fever but this is unusual for mild cases. A sudden change in the bowel habit is common, usually constipation but occasionally diarrhea. Some bleeding may be visible. Absent any local complications (see below), the mainstay of treatment is broad spectrum antibiotics. Most people can be treated outside the hospital with oral antibiotics. More severe presentations or those with complications may need hospital admission and intravenous treatment. During acute attacks of diverticulitis we recommend a diet that is low in fibre with plenty of fluids while the inflammation in the bowel wall settles. See more about diet in diverticulitis here. The primary diagnostic tool for the patient suspected of having acute diverticulitis is a CT scan. This has a very high level of sensitivity for the diagnosis and is the only imaging test that can accurately find or exclude complications. We do not use ultrasound except in the unusual situation where CT may be not appropriate . Colonoscopy is used to exclude other conditions. The timing of colonoscopy is different in each patient. Those who have already had recent colonoscopy (within 2-3 years) do not necessarily need it repeated.
Complications
- Inflammatory mass (phlegmon) – a larger area of inflammation that develops without an abscess (which is an infected fluid collection). This may result in a mass that can be felt in the abdomen.
- Abscess formation – abscesses form around areas of perforation as the body “walls off” the infection. Small abscesses will resolve with antibiotics and larger abscesses are drained by radiologists using an ultrasound or CT machine with a needle and drain. Here at NRGH, our interventional radiologists have extensive experience with this sort of procedure. Surgery acutely for abscess treatment is only required rarely.
- Perforation – the size of a perforation will determine treatment. Small localized perforations where it is confined to the immediate bowel wall area will often be treated with antibiotics without surgery being required. At the other end of the spectrum large perforations with extensive contamination of the abdominal cavity require surgery and may require a colostomy temporarily. The management of each patient is individualized.
- Bowel obstruction - This can be acute or chronic and is often a reason for surgery.
- Fistula formation – this is a rare complication of diverticulitis where the inflammation produces an abnormal connection to a neighboring organ. This is most frequently to the bladder or vagina. This will require surgery in almost all cases.
- Bleeding - Diverticular bleeding is the most common cause of admission to hospital for larger volume rectal bleeding. The bleeding is usually painless and can vary in volume. The majority of bleeding stops spontaneously but colonoscopy is indicated to exclude other causes of bleeding. In a small percentage of cases the colonoscopy may be required to stop the bleeding. Emergency surgery for bleeding alone is only very rarely required.
Surgery
The majority of patients will never require surgery for this condition. Surgery is indicated to treat complications of the disease and may be required acutely or more chronically depending on the circumstances.
Acute surgery may be required if there is a perforation, acute obstruction, ongoing bleeding or an abscess that cannot be drained percutaneously. This may be done laparoscopically or open depending on a number of factors. The need for a colostomy bag has significantly declined in recent years but there are still situations where an intestinal stoma is required; usually only temporarily.
Chronic or interval surgery may be suggested where repeated attacks of diverticulitis are occurring despite treatment. Recurrent attacks may also result in chronic obstruction which will not be improved with antibiotics.
Acute surgery may be required if there is a perforation, acute obstruction, ongoing bleeding or an abscess that cannot be drained percutaneously. This may be done laparoscopically or open depending on a number of factors. The need for a colostomy bag has significantly declined in recent years but there are still situations where an intestinal stoma is required; usually only temporarily.
Chronic or interval surgery may be suggested where repeated attacks of diverticulitis are occurring despite treatment. Recurrent attacks may also result in chronic obstruction which will not be improved with antibiotics.
Colonoscopy
Colonoscopy is indicated in suspected diverticulitis to confirm diverticular disease and to exclude other conditions that may be present (Eg. colon cancer or inflammatory bowel disease). We recommend that the acute inflammation is settled to some degree before undergoing colonoscopy. For more information on colonoscopy click here./colonoscopy.html
Diet
There is a great deal of dietary misinformation with respect to diverticular disease. In general, a high fibre diet is recommended for prevention. Seeds and nuts are often excluded but they are perfectly safe to eat for patients with diverticular disease. A sensible discussion on diet and diverticular disease can be found here. More information on dietary fibre can be found here